Abstract
As the coronavirus disease 2019 (COVID-19) pandemic has spread, so has the psychological impact of the disease been felt worldwide. Among the various types of psychological problems that are caused by COVID-19, anxiety poses a great threat to the physical and mental health of children and adolescents. With an aim of advancing the current work of diagnosing and treating child and adolescent anxiety as a result of the COVID-19 pandemic, this chapter discusses this noticeable global health issue focusing on the following key parts: possible etiology, clinical characteristics, diagnosis and available therapeutic options.
Keywords
- COVID-19
- anxiety
- mental disorders
- child and adolescent
1. Introduction
The COVID-19 pandemic has led to a huge global health crisis, including mental and psychological problems in children and adolescents. Since their physical and mental aspects are not fully developed, they are more susceptible to psychological problems and mental disorders associated with the COVID-19 pandemic [1]. Among the various types of psychological problems and mental disorders caused by COVID-19, anxiety poses a great threat to the physical and mental health of children and adolescents.
Compared to generalized anxiety disorder, child and adolescent anxiety derived from the COVID-19 pandemic has clear inducing factors that are closely correlated with the development of the pandemic, and thus has its unique characteristics. During pandemic prevention and control, limitations in diagnostic and therapeutic options have a huge impact on the physical and mental health, as well as social functions of children and adolescents. Therefore, can it be classified as a new disease? What are the possible explanations for its emergence? What are the main clinical features of this disease? When the disease occurs, do we have a complete diagnosis and treatment system to deal with limitations of the scope of medical activities in special periods? For similar anxiety problems caused by public health emergencies, can we learn from this incident and improve on response measures?
1.1 Child and adolescent anxiety as a result of the COVID-19 pandemic
Anxiety is a normal emotional experience for children and adolescents. It helps in improving their adaptability and coping skills in daily life. However, when anxiety lasts for too long or when anxiety is too serious resulting from some stress factors, which exceeds the reaction of normal children of the same age, children cannot freely recover from long lasting anxiety, and it seriously affects their daily life. Such anxiety is pathological, referred to as anxiety disorder [2]. Using current diagnostic systems (including ICD-10 and DSM-5), children and adolescents with anxiety disorders can be grouped into two. Those grouped as adults include those with generalized anxiety disorders, panic disorders, obsessive–compulsive disorders and so on. The second grouping involves disorders that only occur in children, and they belong to the childhood emotional disorders (F93) in ICD-10, such as childhood dissociative anxiety disorder, childhood phobic anxiety disorder, childhood social anxiety disorder and etc. Selective silence is also included in DSM-5. There are many typical characteristics of COVID-19 associated anxiety disorders in children and adolescents. However, there are no appropriate and effective diagnostic approaches or therapeutic options. Therefore, child and adolescent COVID-19 associated anxiety can be defined as an anxiety disorder that occurs in the context of major public health emergencies, and develops as a result of the pandemic. It is characterized by a series of anxiety symptoms and behavioral problems that are directly or indirectly induced by large-scale public health emergencies, which seriously affect physical and mental health, learning, life as well as communication abilities of children and adolescents. Disease outcomes differ among people, some patients may self-heal, and through intervention, can quickly eliminate anxiety symptoms. Other patients may develop severe mental symptoms, including depression and suicide, as the condition progresses. The disease course is persistent, but may intermittently fluctuate as quarantine measures of covid-19 change (Figure 1). Disease diagnosis and treatment should be simple, accurate, efficient and with a wide reach for large-scale public health emergencies. Regarding the disease, there are more prominent features in children’s normal development, rather than their own abnormalities, so it is different from adult neurological diagnosis. The significance of classifying COVID-19 associated child and adolescence anxiety in childhood mood disorders is worthy of discussion.
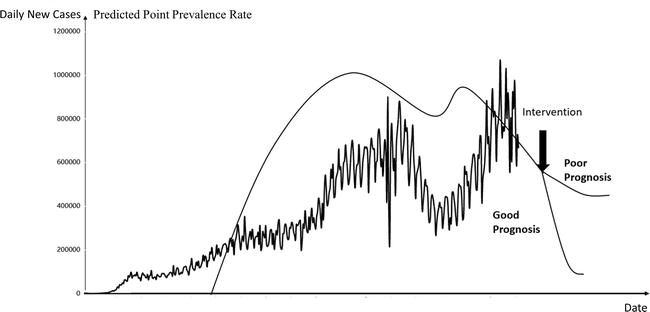
Figure 1.
Prediction of disease development trend.
Next, the possible etiology, characteristics, diagnosis and therapeutic options for COVID-19 associated child and adolescent anxiety are discussed.
In the figure, the irregular curve represents the development trend of the COVID-19 pandemic, the smooth curve represents the predicted development trend of the Child and adolescent anxiety as a result of the COVID-19 pandemic, the abscissa represents time, the ordinate represents the daily new cases of the COVID-19 pandemic and the predicted point prevalence rate of the Child and adolescent anxiety as a result of the COVID-19 pandemic (Figure 2).

Figure 2.
Child and adolescent anxiety as a result of the COVID-19 pandemic.
2. Potential mechanisms
2.1 Temperament
Temperaments are stable psychological characteristics associated with the intensity, speed, flexibility and directivity of psychological activities. Differences in human temperament are congenital and are correlated with nervous system processes [3]. Individuals who cry too much and are too active in infancy are introverted, cautious, shy, timid and unwilling to accept the new environment in childhood. These children, with behavioral inhibition temperaments, often exhibit behavioral characteristics of “inhibition, avoidance and timidity” in the face of life challenges [4]. During the pandemic, implementation of measures such as home isolation is associated with great changes in children’s lifestyle. Children with behavioral inhibition temperament are often very uncomfortable and prone to anxiety [5].
2.2 Pressure and response
Lazarus and Folkman were of the opinion that stress is a kind of psychological state that is caused by specific connections with any environment [6]. When environmental pressure exceeds the range that an individual can bear, he must mobilize other resources to deal with it. Coping has three characteristics: i. Coping is a quality; ii. Coping is a process and iii. Coping is a resource. Quality means that people always respond to the environment in a similar way; process refers to people’s cognitive and behavioral efforts in dealing with all kinds of harmful environmental effects beyond their personal coping resources, and these efforts are constantly changing while resource refers to the condition or internal quality of people to reduce their sense of stress or improve their coping behaviors. When children face stressors, they often resort to coping strategies. Coping strategies are a series of purposeful, conscious and flexible strategies that are aimed at adjusting cognition, emotion and behavior. They are situational and unstable. During continuous coping, people constantly adjust their coping strategies, constantly update and repair themselves, internalize the cognitive experience into coping resources, so as to quickly balance the pressure of the environment in the process of coping to achieve adaptation [7]. When external environmental pressure is too big, an individual cannot develop efficient coping strategies and the balance between the inner mind and environmental pressure cannot be maintained. Therefore, there will be internalization disorders (also known as emotional disorders), and an individual will develop anxiety. For children and adolescents, the COVID-19 pandemic is a stressor whose coping process is associated with great challenges [8]. The uncontrollable spread of the disease has enhanced unpredictability of stressors. Young children have little experience in public health emergencies; therefore, they are unable to adjust their actions by using the experience of dealing with similar situations. Continuous changes in national pandemic prevention policies make it impossible for young children to make corresponding plans to adjust their own handling of stressors. The home isolation policy limits the support provided to children. In this case, it is difficult for children to balance the environmental pressure, and thus the stable emotion is broken, leading to elevated anxiety levels, which has a significant impact on their own social functions and seriously affects their physical and mental health [9].
2.3 Psychoanalytic theory
According to Freud’s view of personality development, personality consists of “Id, Ego and Superego”. “Id” is the most primitive and instinctive part of personality. It includes instinctive drive and repressed habit tendency. The younger the age, the more important the role of “Id”. “Ego” is part of consciousness structure. As children grow older, they consider the consequences and the role of reality. “Superego” represents the moral standard and advanced direction of human life [10]. When a disease is prevalent, children will have a sense of fear when facing a real threat of infection risk. Under strict epidemic prevention conditions and changing living habits, the needs of the Id are repeatedly suppressed, and those may trigger the child’s internal immature defense mechanism. Defense mechanisms are unconscious strategies whereby people protect themselves from anxious thoughts or feelings [11]. However, when this defense mechanism deviates from the logical method of consciousness, it is abnormal psychology. For children who are mentally immature, this defense mechanism is obviously more prone to deviation, the needs of the Id always clash with the needs of the Superego, and the defense mechanism cannot alleviate children’s internal conflicts, which leads to anxiety [12].
2.4 Environmental factors
The pressure brought about by the pandemic does not only affect children, but parents too. For families with poor parenting environments, mental illnesses or emotional problems, special pandemic prevention requirements increase the contact time between parents and children, and bad family relationships predispose children to anxiety [13]. In addition, children’s social communication at this time lacks authenticity, effectiveness, timeliness, and their social support structures are greatly reduced [14], which predisposes them to anxiety.
2.5 Others
The government’s home restriction guidelines during the pandemic may lead to decreased activities of children and adolescents. Lack of exercise, sedentary life style, long-term screen exposure and other problems can easily lead to declined cardiopulmonary functions in children and adolescents [15]. Moreover, information on social media regarding pandemic prevention and control exposes children to a large quantity of information [16, 17]. If there is no correct guidance, children and adolescents are prone to over cognition, and blindly express their discomfort with the new coronavirus, resulting in panic and anxiety.
3. Clinical features
Studies on COVID-19 associated psychological problems among child and adolescents show that anxiety is common among child and adolescents, especially in some specific groups, such as pre-pandemic maltreated adolescents [18]. Since the language system of young children is not perfect, their anxiety is expressed through psychomotor symptoms caused by the limitation of their activities, such as fidgeting, irritability, poor temper control, continual crying, frequent conflict with their families, difficulties in concentration and etc [19]. For relatively older school-age children and adolescents, a series of factors such as school closure, home isolation and online learning during the pandemic is associated with significant learning lifestyle changes. Children’s anxiety is often manifested as nervousness and involuntary fear. Learning and interpersonal communication problems are particularly prominent and exhibit certain characteristics [20]. For maladjustment of online distance learning, short-term intensive curriculum arrangement leads to increased academic pressure, which makes children show extreme performance such as excessive worry about learning or giving up learning. Long term isolation from crowds at home, reduction of communication opportunities with peers inhibits the development of interpersonal communication skills among children, leading to tension, worry and even escape [21]. The loose schedule of work and rest is associated with changes in the living habits. A huge reduction in the amount of daily activities cause children to show the following symptoms, such as difficulty in falling asleep, easiness to wake up, loss of appetite, defecation habits disorder, fatigue and serious autonomic nervous system disorders, such as palpitations, chest tightness, dizziness, nausea and epigastric discomfort [22], and these symptoms are often persistent. In the normalization stage after the pandemic, children’s sensitivity to interpersonal relationships is often more prominent after returning to school, which shows that they are unwilling to contact and communicate with others. After returning to school and classroom, students may be unable to pay attention in class, and their academic performance may decline. Studies in China have shown that anxiety symptoms in high school students and girls are more obvious [23]. This state often lasts for more than one month after the pandemic. Some children gradually adapt, and return to the normal learning and living state, while others gradually aggravate and develop depressive disorders, resulting in self injury and suicide.
4. Assessment
Due to diagnostic and treatment limitations for COVID-19, the disease should be evaluated at an early stage. The self-rating scale is characterized by simplicity and strong operability, and is especially suitable as a diagnostic tool in special periods. Currently, there is no COVID-19 pandemic related scale. Based on related symptoms, we proposed four-dimensional items, such as degree of influence, anxiety, somatic symptoms, learning and interpersonal relationships to evaluate the disease. The new scale refers to The Screen for Child Anxiety Related Emotional Disorders, SCARED [24] and The Multidimensional Anxiety Scale for Children, MASC [25] and Hamilton Anxiety Scale, HAMA [26] and Self-rating Anxiety Scale, SAS [27]and it still needs a lot of research to verify its reliability and validity.
5. Treatment and management
The management goal of COVID-19 associated child and adolescent anxiety is to find out children’s condition in time and in early stages, and to introduce control measures according to different symptoms. Moreover, there is a need to improve anxiety symptoms of children and adolescents, recover social functions, curb disease development and improve on prognosis. The most appropriate comprehensive therapy involves combining psychotherapy and drug therapy. Among them, CBT cognitive behavioral therapy can be adopted as the psychotherapy, and its operability can be enhanced through structured treatment processes [28], so that it has great therapeutic significance in the closed period of the pandemic.
5.1 Psychotherapy
5.1.1 Health education
Health education especially mental health education, in the early stages of the pandemic reduces the development of anxiety [29]. Children and adolescents who know more about the disease and pay attention to its progress are less likely to develop anxiety. The content of health education should include stressors that may cause stress in children. Children should be taught on disease characteristics, inducing factors, clinical manifestations and treatment measures. In the education process, parents should be encouraged to help their children understand the disease more vividly and concretely, establish a psychological defense mechanism, and reduce incidences of anxiety.
5.1.2 Cognitive behavioral therapy
Due to the particularity of the pandemic, face-to-face psychotherapy is difficult to achieve. Remote psychotherapy should be focused on guiding children to conduct self counseling. Cognitive behavioral therapy, through cognitive behavioral intervention technology, changes individual’s unreasonable ideas to adjust the bad moods and inappropriate behaviors, so as to overcome psychological barriers [30, 31]. The treatment process is relatively easy to carry out through the remote guidance mode. Cognitive behavioral therapy (CBT), such as self-control and self-directed training, is very suitable for structured psychotherapy during the pandemic.
What’s the problem?
Do I have any emotional problems during the pandemic? Do I feel anxious or nervous, when the problems occur? Why do these problems occur? What are the stimulus sources? Am I the only one affected? What will I become if I don’t solve them? Children should be encouraged to ask as many questions as possible and to recall all thoughts and feelings in all problem situations.
What is my goal?
For the current situation, what do I want to change and what do I think is the best solution?
Looking at the problem again. Is there any difference between the current situation and the expected situation? Why is there such a difference? What are my feelings?
Re-recognize self-awareness. Is my self-awareness caused by my negative emotions? Try to avoid negative thoughts, focus on the desired change.
Prepare a plan, consider how to tackle each problem, make a good plan, analyze the possible good and bad things in each plan, and then do it.
How it works.
When the plan is realized, check how it is executed, whether it is feasible and whether it works.
5.2 Medication
By enhancing the role of GABA and its receptors, Benzodiazepines (BDZs) produce the effects of sedation, hypnosis, anti-anxiety, anticonvulsion and muscle relaxation, which are widely used in the treatment of adult anxiety [34, 35]. However, their safety and effectiveness in child and adolescent patients have not been determined [36]. Its main adverse reactions are sedation, de-inhibition (such as attack, irritation), respiratory suppression, movement disorders, withdrawal reactions and so on. There have been fewer reports of drug tolerance and dependence among children, but such drugs are dependent in adults and are not recommended for long-term use [37]. In the COVID-19 pandemic context, home isolation makes it difficult for doctors to assess the actual state of children and adolescents, and the risk of medication is much greater than usual. Therefore, it is necessary to be cautious concerning the use of drugs and it is recommended not to use drugs if it is not an emergency [38]. For children and adolescents who are ineffective or unsuitable for psychotherapy, there is a need to fully assess mental outcomes after BDZs (e.g. Lorazepam) administration, and pay close attention to the presence of adverse reactions. It is advised that the treatment should not exceed 3 weeks in order to prevent the occurrence of drug dependence.
6. Prognosis
Since the disease occurs in the context of major public health emergencies and there are significant inducing factors, therefore, when COVID-19 is controlled, its natural prognosis is relatively good, patients with mild anxiety symptoms have the possibility of complete self-healing but the disease duration is relatively long. Moreover, there is a certain impact on social functions of adolescents and children. In some patients, anxiety symptoms are more serious, and the natural prognosis is relatively poor without timely diagnosis and intervention, and the likelihood of inducing other mental symptoms is greatly increased. Motor restlessness associated with long-term limited activity may lead to attention deficit hyperactivity disorder problems [39], continuous lack of interpersonal communication may lead to the development of social disorders [40], persistent increased anxiety is more likely to induce depression, serious suicidal thoughts and behaviors [41]. All types of outstanding problems continue until the pandemic has been managed, patients cannot return to school or maintain normal living patterns and their social functions continue to be impaired. In contrast, patients who were diagnosed in time, and who had adequate intervention had good prognoses, their anxiety symptoms quickly disappeared, their psychological defense mechanisms were established, and their social functions were restored. Therefore, when such public health emergencies occur, the goal should be early diagnosis, early intervention and follow-up investigations to improve prognosis.
7. Conclusion
Considering the particularity of the incidence and development process of this disease, we believe that the significance of COVID-19 associated child and adolescent anxiety, as a childhood mood disorder is well worth exploring. We have elucidated on the potential factors that may affect the development of the disease from multiple perspectives. In the COVID-19 context, there is a need to develop a new evaluation scale to assess the disease. For prevention and control, cognitive behavioral therapy-based psychotherapy plays a greater role in disease management.
To what extent do you think the covid-19 pandemic has affected your life?
Almost no effect Slight effect Moderate effect Severe effect.
Since the outbreak of the COVID-19 pandemic, have you felt more nervous and anxious than usual?
No/Occasionally Sometimes Often Continues.
Since the outbreak of the COVID-19 pandemic, have you felt scared for no reason?
No/Occasionally Sometimes Often Continues.
Since the outbreak of the COVID-19 pandemic, have you felt in a trance, as if everything around you was unreal when you were afraid?
No/Occasionally Sometimes Often Continues.
Since the outbreak of the COVID-19 pandemic, have you been easily upset or panicked?
No/Occasionally Sometimes Often Continues.
Since the outbreak of the COVID-19 pandemic, do you think you might be going crazy?
No/Occasionally Sometimes Often Continues.
Since the outbreak of the COVID-19 pandemic, have your hands and feet ever trembled?
No/Occasionally Sometimes Often Continues.
Since the outbreak of the COVID-19 pandemic, have you been distressed by headaches, neck pain and back pain?
No/Occasionally Sometimes Often Continues.
Since the outbreak of the COVID-19 pandemic, have you felt easily weak and tired?
No/Occasionally Sometimes Often Continues.
Since the outbreak of the COVID-19 pandemic, have you felt that your heartbeat has been fast?
No/Occasionally Sometimes Often Continues.
Since the outbreak of the COVID-19 pandemic, have you been distressed by dizziness?
No/Occasionally Sometimes Often Continues.
Since the outbreak of the COVID-19 pandemic, have you ever had a fainting episode or felt like you were going to faint?
No/Occasionally Sometimes Often Continues.
Since the outbreak of the COVID-19 pandemic, have you ever felt numbness and tingling in your hands and feet?
No/Occasionally Sometimes Often Continues.
Since the outbreak of the COVID-19 pandemic, have you ever been distressed by stomach pain and indigestion?
No/Occasionally Sometimes Often Continues.
Since the outbreak of the COVID-19 pandemic, do you often feel the need to urinate?
No/Occasionally Sometimes Often Continues.
Since the outbreak of the COVID-19 pandemic, have your hands often been dry and warm?
No/Occasionally Sometimes Often Continues.
Since the outbreak of the COVID-19 pandemic, have you ever blushed and became hot?
No/Occasionally Sometimes Often Continues.
Since the outbreak of the COVID-19 pandemic, have you ever had difficulties falling asleep and often have nightmares?
No/Occasionally Sometimes Often Continues.
Since the outbreak of the COVID-19 pandemic, have you ever felt a headache while studying?
No/Occasionally Sometimes Often Continues.
Since the outbreak of the COVID-19 pandemic, have you ever been unable to concentrate while studying?
No/Occasionally Sometimes Often Continues.
Since the outbreak of the COVID-19 pandemic, have you ever worried that your classmates or peers no longer like you?
No/Occasionally Sometimes Often Continues.
Since the outbreak of the COVID-19 pandemic, are you afraid of returning to school?
No/Occasionally Sometimes Often Continues.
Total score:
*Note:
How to Score
Check that all statements have been answered. Add up the score for each response to get the Total Score.
For item 1
Almost no effect=1 Slight effect=2 Moderate effect=3 Severe effect=4
For item 2-22
No/Occasionally=0 Sometimes=1 Often=2 Continues=3
Interpreting the Score
A Total Score of 15 or above highly indicates child and adolescent anxiety as a result of the COVID-19 pandemic.
References
- 1.
Wang, Q . and R. Xu, et al. (2021). “Increased risk of COVID-19 infection and mortality in people with mental disorders: Analysis from electronic health records in the United States.” World psychiatry : official journal of the World Psychiatric Association (WPA) 20 (1): 124-130. - 2.
Mahdi, M. and S. Jhawar, et al. (2019). “Cognitive behavioral therapy for childhood anxiety disorders: What happens to comorbid mood and behavioral disorders? A systematic review.” Journal of affective disorders 251 : 141-148. - 3.
Slagt, M. and J. S. Dubas, et al. (2016). “Differences in sensitivity to parenting depending on child temperament: A meta-analysis.” Psychological bulletin 142 (10): 1068-1110. - 4.
Thiel, F. and L. Iffland, et al. (2020). “Specific relations of dimensional anxiety and manifest anxiety disorders during pregnancy with difficult early infant temperament: A longitudinal cohort study.” Archives of women’s mental health 23 (4): 535-546. - 5.
Fox, A. S. and N. H. Kalin (2014). “A translational neuroscience approach to understanding the development of social anxiety disorder and its pathophysiology.” The American journal of psychiatry 171 (11): 1162-1173. - 6.
Folkman, S. (2013). Stress: Appraisal and coping. Encyclopedia of Behavioral Medicine. M. D. Gellman and J. R. Turner. New York, NY, Springer New York: 1913-1915. - 7.
Compas, B. E. and S. S. Jaser, et al. (2017). “Coping, emotion regulation, and psychopathology in childhood and adolescence: A meta-analysis and narrative review.” Psychological bulletin 143 (9): 939-991. - 8.
Petrocchi, S. and A. Levante, et al. (2020). “Maternal distress/coping and Children’s adaptive behaviors during the COVID-19 lockdown: Mediation through Children’s emotional experience.” Frontiers in public health 8 : 587833. - 9.
Jones, E. and A. K. Mitra, et al. (2021). “Impact of COVID-19 on mental health in adolescents: A systematic review.” International journal of environmental research and public health 18 (5). - 10.
Luborsky, L. and M. S. Barrett (2006). “The history and empirical status of key psychoanalytic concepts.” Annual review of clinical psychology 2 : 1-19. - 11.
Mihalits, D. S. and M. Codenotti (2020). “The conceptual tragedy in studying defense mechanisms.” Integrative psychological & behavioral science 54 (2): 354-369. - 12.
Mukhopadhyay, P. and S. Tarafder, et al. (2010). “Instinctual impulses in obsessive compulsive disorder: A neuropsychological and psychoanalytic interface.” Asian journal of psychiatry 3 (4): 177-185. - 13.
Saddik, B. and A. Hussein, et al. (2021). “The psychological impact of the COVID-19 pandemic on adults and children in the United Arab Emirates: A nationwide cross-sectional study.” BMC psychiatry 21 (1): 224. - 14.
Sobowale, K. and H. Hilliard, et al. (2020). “Real-time communication: Creating a path to COVID-19 public health activism in adolescents using social media.” Journal of medical Internet research 22 (12): e21886. - 15.
Umutlu, G. and N. E. Acar, et al. (2021). “COVID-19 and physical activity in sedentary individuals: Differences in metabolic, cardiovascular, and respiratory responses during aerobic exercise performed with and without a surgical face masks.” The Journal of Sports Medicine and Physical Fitness. - 16.
Jain, R. and C. A. Kelly, et al. (2021). “A trainee-led social media advocacy campaign to address COVID-19 inequities.” Pediatrics 147 (3). - 17.
Kaess, M. (2020). “Editorial: Social media use in children and adolescents - on the good or the bad side of the force?” Child and adolescent mental health 25 (4): 199-200. - 18.
Guo, J. and M. Fu, et al. (2020). “Is the psychological impact of exposure to COVID-19 stronger in adolescents with pre-pandemic maltreatment experiences? A survey of rural Chinese adolescents.” Child abuse and neglect 110 : 104667. - 19.
Wang, Y. and Z. Hu, et al. (2020). “Changes in network centrality of psychopathology symptoms between the COVID-19 outbreak and after peak.” Molecular psychiatry 25 (12): 3140-3149. - 20.
Schmidt, S. J. and L. P. Barblan, et al. (2021). “Age-related effects of the COVID-19 pandemic on mental health of children and adolescents.” European journal of psychotraumatology 12 (1): 1901407. - 21.
Blake, H. and H. Knight, et al. (2021). “Students’ views towards Sars-Cov-2 mass asymptomatic testing, social distancing and self-isolation in a university setting during the COVID-19 pandemic: A qualitative study.” International journal of environmental research and public health 18 (8). - 22.
Porzionato, A. and A. Emmi, et al. (2020). “Sympathetic activation: A potential link between comorbidities and COVID-19.” The FEBS journal 287 (17): 3681-3688. - 23.
Chen, X. and H. Qi, et al. (2021). “Depression, anxiety and associated factors among Chinese adolescents during the COVID-19 outbreak: A comparison of two cross-sectional studies.” Translational psychiatry 11 (1): 148. - 24.
Birmaher, B. and S. Khetarpal, et al. (1997). “The screen for child anxiety related emotional disorders (SCARED): Scale construction and psychometric characteristics.” Journal of the American Academy of Child and Adolescent Psychiatry 36 (4): 545-553. - 25.
March, J. S. and J. D. Parker, et al. (1997). “The multidimensional anxiety scale for children (MASC): Factor structure, reliability, and validity.” Journal of the American Academy of Child and Adolescent Psychiatry 36 (4): 554-565. - 26.
Hamilton, M. (1959). “THE ASSESSMENT OF ANXIETY STATES BY RATING.” British Journal of Medical Psychology 32 (1): 50-55. - 27.
William, W. K. Z. M. (1971). “A rating instrument for anxiety disorders.” Psychosom 12 (6): 371-379. - 28.
Nordentoft, M. and S. Austin (2014). “CBT for psychotic disorders: Beyond meta-analyses and guidelines - it is time to implement!.” World psychiatry : official journal of the World Psychiatric Association (WPA) 13 (3): 260-261. - 29.
Cerda, A. A. and L. Y. García (2021). “Factors explaining the fear of being infected with COVID-19.” Health Expectations: An International Journal of Public Participation in Health Care and Health Policy. - 30.
Tarrier, N. (2014). “CBT for psychosis: Effectiveness, diversity, dissemination, politics, the future and technology.” World psychiatry : official journal of the World Psychiatric Association (WPA) 13 (3): 256-257. - 31.
Wise, J. (2019). “Depression in children: Offer digital CBT as first line treatment, says NICE.” BMJ (Clinical research ed.) 364 : l364. - 32.
Conway, A. (2020). “Longitudinal associations between parenting and inattention, impulsivity, and delay of gratification in preschool-aged children: The role of temperamental difficultness and toddler attention focusing.” Developmental neuropsychology 45 (5): 309-329. - 33.
Meichenbaum, D. (1977). Self-Instructional Training. Cognitive-Behavior Modification: An Integrative Approach. Boston, MA, Springer US: 17-54. - 34.
Sieghart, W. and M. M. Savić (2018). “International Union of Basic and Clinical Pharmacology. CVI: GABA receptor subtype- and function-selective ligands: Key issues in translation to humans.” Pharmacological reviews 70 (4): 836-878. - 35.
Sigel, E. and M. Ernst (2018). “The benzodiazepine binding sites of GABA receptors.” Trends in pharmacological sciences 39 (7): 659-671. - 36.
Mody, K. and S. Kaur, et al. (2018). “Benzodiazepines and development of delirium in critically ill children: Estimating the causal effect.” Critical care medicine 46 (9): 1486-1491. - 37.
Moreno-Gutíerrez, P. A. and A. Gaviria-Mendoza, et al. (2020). “Long-term users of benzodiazepines in Colombia: Patterns of use and cessation of treatment.” Drug and alcohol dependence 210 : 107962. - 38.
Kuang, H. and J. A. Johnson, et al. (2017). “The efficacy of benzodiazepines as acute anxiolytics in children: A meta-analysis.” Depression and anxiety 34 (10): 888-896. - 39.
Liu, J. B. and Z. P. Xue, et al. (2020). “[Moderated mediation analysis for symptoms of attention deficit/hyperactivity disorder with the symptoms of anxiety in children].” Zhongguo dang dai er ke za zhi = Chinese journal of contemporary pediatrics 22 (7): 768-773. - 40.
van Niekerk, R. E. and A. M. Klein, et al. (2017). “The role of cognitive factors in childhood social anxiety: Social threat thoughts and social skills perception.” Cognitive therapy and research 41 (3): 489-497. - 41.
Duffy, M. E. and J. M. Twenge, et al. (2019). “Trends in mood and anxiety symptoms and suicide-related outcomes among U.S. undergraduates, 2007-2018: Evidence from two National Surveys.” The Journal of adolescent health: official publication of the Society for Adolescent Medicine 65 (5): 590-598.